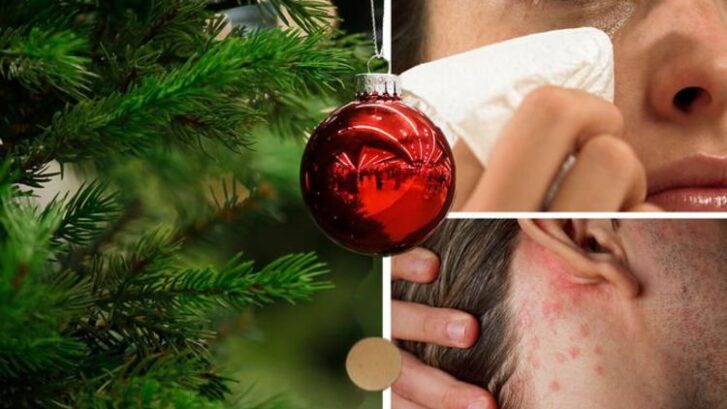
Could You Be Allergic to Your Holiday Tree?
What is Christmas Tree Syndrome?
Christmas tree syndrome refers to an allergic reaction that some people experience after bringing a Christmas tree into their home. This syndrome can cause a variety of symptoms, including wheezing, sneezing, coughs, sore eyes, and potentially serious asthma attacks. Interestingly, both real and artificial Christmas trees can trigger these allergic reactions.
Causes of Christmas Tree Syndrome
- Real Trees: Trees like cypress and pine can accumulate high amounts of pollen from other plants before they are cut down. Additionally, Christmas trees can carry about 50 different types of mold, which can increase the mold spore count in a home by more than six times.
- Artificial Trees: These can also be problematic if they gather dust, dust mites, or mold while in storage.
Who is Affected?
Christmas tree syndrome is more common in people prone to allergies and asthma but can affect anyone. The symptoms are particularly noticeable for those who regularly bring real trees into their homes during the holiday season.
Managing Christmas Tree Syndrome
- For Real Trees:
- Hose down the tree before bringing it indoors to wash off allergens.
- Shake the tree to remove loose debris and rinse it with a hose or veggie wash, drying it thoroughly afterward.
- Consider less allergenic trees like fir, spruce, or cypress, especially the Leyland Cypress, which does not produce pollen.
- For Artificial Trees:
- General Tips:
- Use air purifiers in the room with the tree to trap allergens.
- Clean and unpack Christmas ornaments and decorations outside to reduce dust and mold exposure.
- If allergies persist with both live and artificial trees, consider setting up a decorated tree outside a patio door or large window to enjoy it from indoors.
- Health Precautions:
Christmas tree syndrome, while not widely known, can significantly impact the quality of life during the holiday season for those susceptible. By understanding its causes and implementing these management strategies, you can enjoy your festive decorations without compromising your health. Remember, if symptoms persist, consult a healthcare professional for personalized advice and treatment.