‘What’s the Harm?’ Possibly a Great Deal
Our concierge doctors understand the desperation and fear that people are feeling as a result of the novel coronavirus. We’re worried that if we or our loved ones catch it, there won’t be a cure.
These feelings are real, understandable, and normal. Unfortunately, they can give rise to false hopes and a willingness to try anything. This natural tendency has resulted in a number of laymen repeating the refrain, “What’s the harm?” in trying different unproven drugs to combat the virus.
The response to that question is, possibly a great deal.
The hydroxychloroquine question
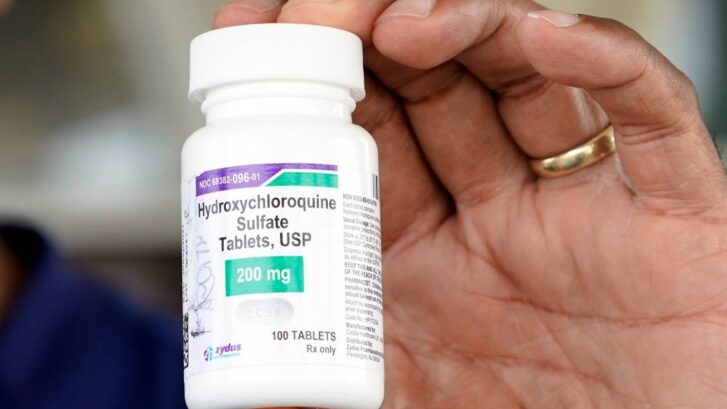
Let’s take the example of the most well-known of the drugs that has been proposed as a possible treatment for COVID-19, hydroxychloroquine (HCQ).
Used for years to treat the debilitating symptoms of malaria, it is also prescribed to decrease the symptoms of rheumatoid arthritis, scleroderma, and sarcoidosis, among other diseases. It’s especially important to those who have lupus, an autoimmune disorder in which some people’s immune system, for some unknown reason, flips into overdrive, causing such symptoms as fever, extreme fatigue, photosensitivity, painful or swollen joints and muscle pain, and swelling in the legs.
Because of the recent publicity surrounding HCQ, these patients are already experiencing a shortage of the drug they need to be able to live a normal life.
But proponents continue to push for widespread use of this drug, arguing that because it’s been around for decades, it can’t do any harm to take it.
Side effects trigger restraint
Tom Hanks’ wife, the singer and actress Rita Wilson, disagrees. Both stars were infected with COVID-19 while in Australia in March for a film Hanks was making, and both contracted the disease.
One of the drugs used to treat Wilson at Gold Coast University in Queensland was hydroxychloroquine.
“I don’t know if the drug worked or if it was just time for the fever to break,” she told CBS This Morning. “My fever did break but the chloroquine had such extreme side effects . . . I was completely nauseous, I had vertigo, and my muscles felt very weak . . . I think people have to be very [cautious] about that drug.”
Last week, the Australian Health Protection Principal Committee—the country’s expert panel on health emergencies—recommended against using the drug in hospitals due to its side effects.
Earlier this month, London’s Daily Mail reported that Swedish hospitals had also abandoned its use in coronavirus patients after reports it was causing blinding headaches, severe cramps, and vision loss. Britain, saying there is “no strong evidence” the drug could effectively treat COVID-19, will not allow doctors there to prescribe it to patients.
The most extreme side effect: death
So, some might wonder, what are a few “extreme side effects” when your life is at stake? Possibly your life. Most people who contract COVID-19 survive the illness, especially if it’s not a severe form. But would that be the case if they had been given unproven medication such as HCQ?
According to USA Today, “The drug label for HCQ, and its close relative chloroquine, is very clear about the risks; both contain a page-and-a-half of stark warnings that include:
- the possibility of blindness due to retinal injury;
- loss of consciousness due to low blood sugar;
- suicidal behavior;
- heart failure;
- potentially lethal interactions with other drugs;
- lethal heart rhythm disturbances; and, yes,
- death”
But if you’re already on the verge of death, what do you have to lose, the thinking goes. That might be a logical—even compelling—argument, except that numerous clinical trials of have never found that HCQ is effective against any type of virus.
You could use the same argument for trying antibiotics on colds and the flu, except . . . same problem. Antibiotics kill bacteria, not viruses, and the side effects and long-term damage of antibiotic overuse are well documented.
Where did the idea arise?
So why the clamor for HCQ to combat COVID-19? Because it is an immune modulator; that is, it depresses the immune system, preventing the body’s overreaction to triggers such as the coronavirus, a process that is thought to be responsible for many of the COVID-19-related deaths.
And, indeed, it may ultimately prove useful in the fight against the novel coronavirus, which is why a number of clinical trials are underway around the world and in the United States to test its efficacy in severe cases, including at the National Institutes for Health (NIH).
But as a drug to be prescribed to prevent the disease or to treat mild cases? No. Not at this time, when the known dangers far outweigh any proven benefit.
Other drugs show promise
The same is true for several other rumored preventatives or cures, including the parasite drug ivermectin, which has been the subject of a recent social media craze, or remdesivir, an anti-viral-drugs.com. Both of these drugs are also currently in clinical trials because they have shown a great deal of promise when used around the world in COVID-19 patients, much more so than has hydroxychloroquine.
It’s important to remember that any drug, whether prescribed or over-the-counter (OTC), has the potential for side effects, some of which can be serious and even deadly.
Another popular saying has arisen lately in another context: “Don’t let the cure be worse than the disease.” In the context of throwing untested and unproven drugs at a disease we still know very little about, this is a good axiom to keep in mind.
Please consult with us if you have any questions or concerns about COVID-19.
Meanwhile, the best “treatment” at this time is still prevention: staying at home as much as possible, frequent hand washing, and social distancing of six feet or more if you must go out.